The connection between the gut and brain offers clues to improved management of mental health and mood disorders.
Gut bacteria are known to help produce neurotransmitters, hormones, and neuropeptides – and these compounds are able to cross-talk with the brain in direct and indirect ways (1).
While we’ve been inundated with information on prebiotics and probiotics – there is increasing chatter about postbiotics.
Postbiotics are the metabolic byproducts of healthy flora that exert effects in the gut and the entire body. They’ve been referred to as “metabolites” from the gut – and the entire diversity of metabolites has been referred to as the “metabolome”.
If you’re like me, the concept of “postbiotics” is easier to understand and wrap your head around.
Postbiotic compounds can be antimicrobial, prebiotic, anti-inflammatory, immune-modulating, and they can also be hormonally active. Many of your neurotransmitters are actually produced in the gut – and communicate to the brain and surrounding body via the bloodstream.
As a result – healthy bacteria in the gut help regulate inflammation, brain function, nerve health, appetite, and more.
Spore Probiotics and Depression
 Recently, a randomized double-blind trial looked at 40 patients with Major Depressive Disorder. The treatment group received a spore-forming Bacillus coagulans supplement over 90 days.
Recently, a randomized double-blind trial looked at 40 patients with Major Depressive Disorder. The treatment group received a spore-forming Bacillus coagulans supplement over 90 days.
After the 90 days the B. coagulans treatment group reported significant decreases in depression, as well as improvements in the quality of life and quality of sleep (2).
The researchers proposed the findings may have been due to the ability of spore-forming bacteria like B. coagulans and others to increase in short-chain fatty acid (SCFA) production. SCFA’s are regarded for their anti-inflammatory properties and the ability to support gastrointestinal and immune health.
SCFAs are among some of the most important postbiotics known currently.
Additionally, Bacillus subtilis, another spore-forming bacteria, may help support serotonin synthesis by supporting the production of the amino acid precursor tryptophan (3; 4). Tryptophan levels in the gut are correlated with serotonin levels in the brain.
If you’ve ever heard of 5-HTP (5-hydroxy-tryptophan) – this is a derivative of tryptophan and happens to be a direct precursor to serotonin production in the body (along with the help of vitamin B6).
Interestingly, serotonin is not just a mood hormone, but it plays roles in gut motility, cardiovascular health, and sexual function.
By supporting serotonin activity, all of these areas inside and outside of the brain are also supported.
The serotonin link has been discussed in animal studies as well. A study with chickens reported less aggressive behavior and higher serotonin levels in hens receiving B. subtilis supplementation.
While it can be difficult to translate these findings to humans, much of the neurotransmitter physiology is conserved across species.
It’s important to note that if taking antidepressants – be mindful of taking any direct serotonin supports like 5-HTP and Tryptophan and cross-check your intended protocol with your prescribing professional.
Depression as Brain Inflammation – Leaky Gut and Bacillus Probiotics
 Disruptions of the gut barrier lead to higher absorption of inflammatory lipopolysaccharides (LPS) – creating bursts of metabolic endotoxemia.
Disruptions of the gut barrier lead to higher absorption of inflammatory lipopolysaccharides (LPS) – creating bursts of metabolic endotoxemia.
Inflammatory messengers known as cytokines increase in response to higher levels of these LPS toxins in the blood.
The model of depression has evolved much more beyond serotonin dynamics – but into a “Cytokine Model of Depression”. This model has now been around for at least two decades with increasing support – but unfortunately, it can take over twenty years for old models to adapt and change. LPS levels in the blood (due to leaky gut) may be a specific trigger of depression (5)
It’s important to understand that brain problems can be due to general “inflammation” and that brain inflammation can come from the gut.
I recommend checking out A Mind of Your Own by Dr. Kelly Brogan – she’s been at the forefront of a functional approach to depression, with arrows in her back to prove it. It hasn’t been easy to promote a new model that points blame at some powerful industries who have strong stakes in an incomplete serotonin or neurotransmitter model of depression.
While the book title is targeted to women – the principles are not gender-specific.
If you’re analytical-minded, Dr. Brogan also co-authored a highly-referenced textbook with Dr. James Greenblatt on the subject that I think is worthwhile Integrative Therapies for Depression: Redefining Models for Assessment, Treatment and Prevention – it bridges clinical and academic discussions from experts in the field.
Low Inflammation + Time = Chronic Disease
Low levels of gut-derived toxins in the blood over time contributes to the progression of a number of chronic diseases.
Here’s a quick summary on how leaky gut leads to depression and other brain symptoms…
1.) Leaky gut is due to holes in the cheesecloth lining of the gut. “Leaky brain” is when there are holes or tears in the finer cheesecloth of the blood brain barrier. Triggers can be stress, head trauma, flora imbalance, food sensitivities (wheat and dairy as biggest culprits), infection, parasites, and more)
2.) When “leaky brain” exists, toxins cross the blood-brain-barrier – initiating an immune response by glial cells. Glial cells are like bazooka-carrying infantry who will shoot at a mouse the same way it might a war-ship. The brain’s immune system is not designed to expect man-made chemicals in its realm – so it assumes the issue is serious when faced with these “new” invaders. This is why gluten and other food sensitivities can lead to balance issues, mental fog, and forgetfulness! And you’re MUCH more likely to have brain symptoms from a gluten problem – than having gut problems.
3.) With this overactivated immune response – collateral damage occurs to otherwise healthy neurons and brain pathways.
4.) Over time, the tissue damage and unnecessary cell death adds up and symptoms may develop. The body produces antibodies to its own tissues and can start attacking healthy tissue.
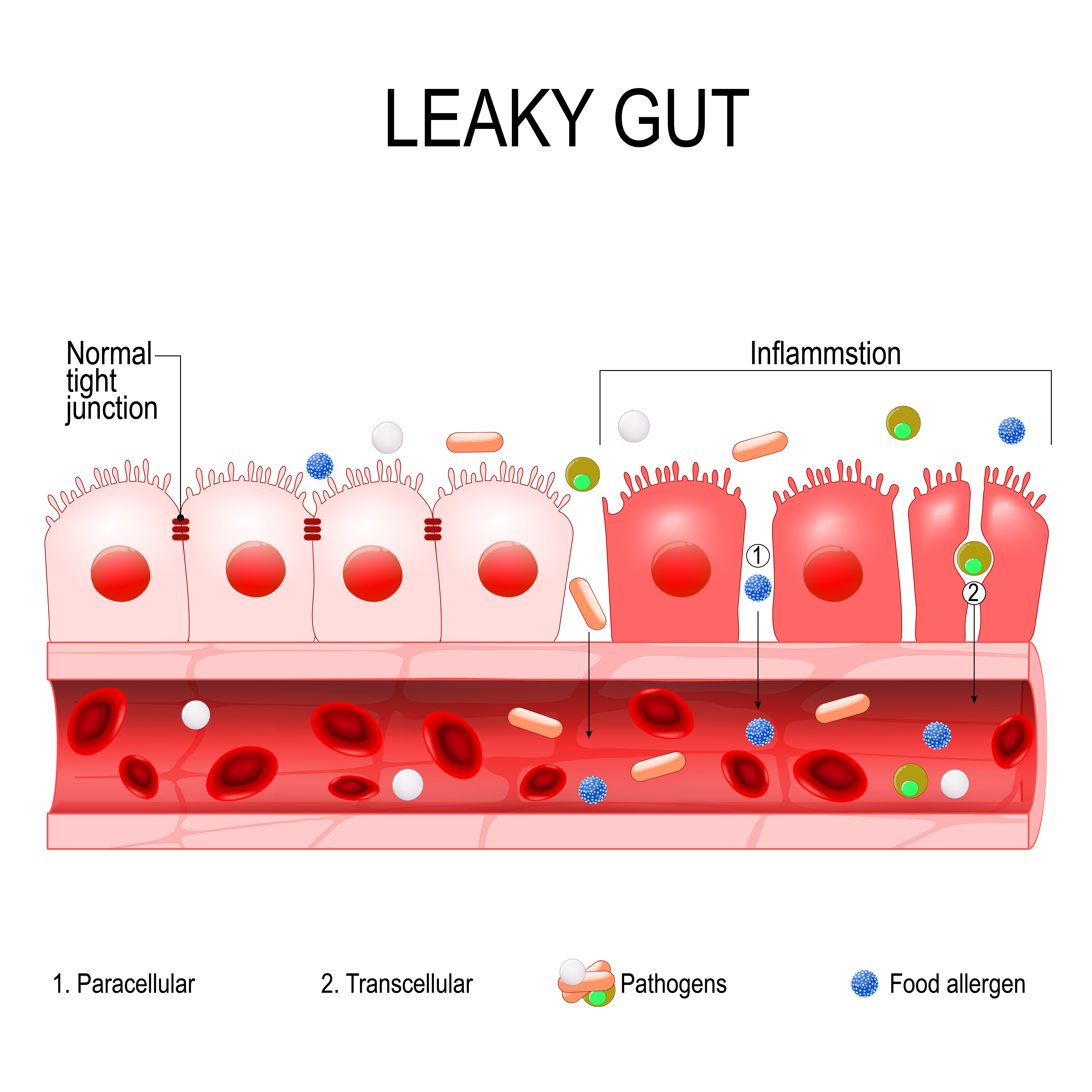
New studies report the ability of a combination of Bacillus subtilis, B. indicus, B. licheniformis, and B. clausii to reduce leaky gut and to limit the ability of inflammatory LPS to cross the blood-brain barrier (6) – Thus, mitigating this entire inflammatory sequence at its roots.
This combination of Bacillus organisms is known commercially as Megasporebiotic.
Supplementation with spore probiotics may also help boost other healthy groups of flora – especially when combined with prebiotic oligosaccharides. (7)
I use Megasporebiotic as my source of spore probiotics – and it remains the most popular supplement used in my practice and store. Spore probiotics are unique in that normal levels in your body depend on routine exposure to these Bacillus microbes.
The body normally supplies is its needs by interacting with dirt in your environment. As most of us live very sanitary lives – supplementation is arguably the next best option – although some fermented foods like Saurkraut or Natto will often use B. coagulans or B. subtilis as the culture of choice.
Megasporebiotic can be combined with RestorFlora and HU58 to maximize the benefits of Bacillus microbes and to support gut dysbiosis. Restorflora is known for its yeast balancing benefits, and HU58 contains a high potency Bacillus subtilis that is known to product the most natural antimicrobial compounds to help crowd out overgrown bacteria – such as in the small intestine.
I generally take a Bifidobacteria probiotic like Trubifido or broader flora support like Theralac in addition to spore probiotics so that I support diversity in the small and large intestines equally.
If I had to choose to take one, I would go with Megasporebiotic, as Bacillus organisms engage in social behavior known as quorum sensing (8). In summary, quorum sensing allows Bacillus microbes to invite healthy bacteria and ward off bad guys by releasing communication signals amongst the colony.
Moreover, you can support Bifidobacteria and Lactobacilli naturally with the diet – unless you’re eating dirt or food off the ground, you’re likely not getting enough spore probiotics.
Prebiotics taken as supplements will also support the diversity of these non-spore strains long-term.
Gut, Brain, Energy, and Inflammation Support Work Together
For inflammation support, some of my favorites are Curcumin and Palmitoylethanolamide (PEA).
I also commonly use lion’s mane mushroom, phosphatidylserine, and phosphatidylcholine when supporting the brain.
Nerve tissue is also highly rich in mitochondria – which produce the energy fuel necessary for proper function. If the mitochondria are not firing on all cylinders – brain function is often the first place you’ll see it.
NAD+ is the “currency” that helps regulate your metabolism – niacin, and specifically, nicotinamide riboside (known as Truniagen) directly supports NAD+ production in the brain and is associated with brain health.
A gluten-free diet also goes a long way to support strong gut and brain barriers. Dairy-free is also a strong recommendation as well. Both gluten and dairy are common triggers of leaky gut – triggering toxin absorption into the blood, triggering inflammation that can lead to brain symptoms like anxiety and depression.
- A mini-protocol to support the brain will include aspects to support leaky gut, increase microbiome diversity, quell inflammation, support blood flow, and boost brain energy.
- Let’s not forget the power of sunlight exposure as well as daily gratitude and meditation practice – which are implemented independently from outside support at no extra cost aside from as little as five minutes per day over a minimum of eight weeks.
As the nervous system is the master controller of all body activities – a focus on the brain and gut arguably improves aspects of all physiology – as well as a secondary benefit on your ability to initiate and maintain healthy lifestyle habits.
Related Resources:
- Megasporebiotic Complete Resource Guide
- Roaring Benefits of Lion’s Mane Mushroom
- Gut and Inflammation – New Targets to Manage Depression Naturally
- How to Stop Your Gut From Leaking Toxins into Your Blood
- Megasporebiotic and Leaky Gut Study
- Understanding Leaky Gut, Autoimmunity, and Beyond
- Health Benefits of Bacillus Spore Probiotics
- Megasporebiotic and Megaprebiotic Synbiotic – Spores and Oligosaccharides Study
- Discover the Benefits of Palmitoylethanolamide (PEA)
- “Fountain of Youth” Benefits of Nicotinamide Riboside – a New Form of Vitamin B3
- The Many Health Benefits of Short Chain Fatty Acids
- What are the Health Benefits of Turmeric?
- Following a Gluten-Free Diet? Make Sure You Read this So You Don’t Make this Key Mistake…
- B. longum 1714 Benefits
Related Books:
- You Can Fix You Brain – Dr. Tom O’Bryan (my most highlighted book of 2019!)
- A Mind of Your Own – Dr. Kelly Brogan
- Integrative Therapies for Depression: Redefining Models for Assessment, Treatment and Prevention – Dr. James Greenblatt and Dr. Kelly Brogan
- Why isn’t My Brain Working? – Dr. Datis Kharrazian