Discover how to navigate histamine intolerance, from low-histamine diets to DAO supplements, so you can build your personalized plan, enjoy meals without fear, and reclaim your energy.
Picture this: You eat a healthy dinner—maybe last night’s leftover salmon and a fresh spinach salad. But instead of feeling energized, your head starts pounding, your skin feels hot and flushed, and a wave of anxiety or nausea hits. It just doesn’t make sense.
Your friend had the exact same meal and feels totally fine.
What gives? You’re not imagining it. These confusing symptoms could be your body’s way of signaling a histamine issue, a natural chemical you can’t see or taste. It’s not an infection or a typical food allergy, but a tipping point—like a bucket that overflows.
For most people, this “histamine bucket” drains easily. But for some, the bucket fills too quickly, or the drain clogs. When it overflows, it can trigger a confusing cascade of symptoms that seem unrelated: headaches, stomach cramps, itchy skin, debilitating brain fog, or a racing heart. Doctors often miss the connection because these issues span multiple specialties, leaving you with a pile of disparate diagnoses but no real answers.
This is the hidden, frustrating reality of histamine intolerance. It’s more than a collection of physical symptoms; it can be a thief of joy and connection.
It’s the anxiety that turns every meal into a calculated risk. It’s the isolation you feel when you have to bow out of a dinner party or can’t share a glass of wine with friends. It’s the exhaustion of explaining an “invisible illness” that others can’t see but dominates your daily life.
You start to question your own experience: “Is this just in my head?”
Here is the crucial truth: It is not.
Your symptoms are real, and their root cause is physical. The good news is that once you understand the mechanics of the bucket—how it fills and how it drains—you gain the power to fix it. You can stop managing isolated symptoms and start solving the core problem to reclaim your comfort, energy, and freedom around food.
Let’s unravel the mystery.
What is Histamine Intolerance? (It’s Not an Allergy)
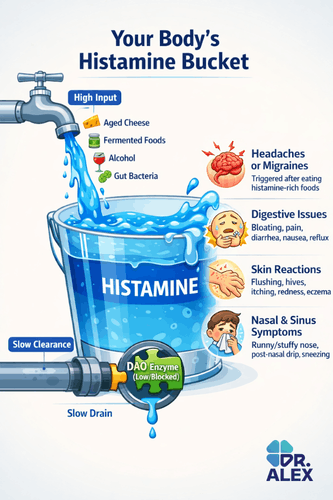
So, what’s actually going on?
Let’s stick with the bucket idea. Imagine your body has a bucket for a natural chemical called histamine.
Histamine isn’t bad. In fact, it’s essential. It’s a messenger that helps your immune system fight real threats, tells your stomach to digest food, and wakes up your brain. It’s like the water in your bucket—you need it to function.
The problem happens with balance.
For people with histamine intolerance, two things go wrong:
- The faucet is on too high (too much histamine coming in). This can be from high-histamine foods (such as aged cheeses, fermented foods, and leftovers), from drinks like alcohol, or even from bacteria in your own gut producing too much of it.
- The drain is clogged (your body can’t clear it out fast enough). This is usually the main issue. Your body uses a special enzyme, mainly called Diamine Oxidase (DAO), to break down and drain histamine from your system. If you don’t produce enough DAO, or something blocks it, the drain clogs.
When the bucket overflows, that’s histamine intolerance. The excess histamine floods your system and causes all sorts of confusing symptoms in your gut, skin, brain, and heart.
Here’s the critical part: This is NOT a food allergy.
- A classic allergy (like to peanuts or shellfish) is like your immune system seeing a harmless peanut as a bomb and hitting the panic button—releasing massive amounts of histamine all at once. This is an immediate, severe, and specific reaction.
- Histamine intolerance is a chemical imbalance. It’s a slower, cumulative overflow from your everyday bucket. It’s not your immune system attacking one specific food or toxin; it’s your body struggling to manage the total load of a chemical that’s already in many different foods and drinks.
Think of it this way: An allergy is a faulty alarm system. Histamine intolerance is a plumbing problem.
Understanding this difference is the first, crucial step to finding real relief. It means the solution isn’t about avoiding one or two “allergens,” but about learning how to turn down the faucet and unclog the drain.
What Histamine Does In Your Body (And Why It Backfires)
Let’s meet the main character: histamine.
It’s a tiny chemical, but a major multitasker in your body. The key is understanding that histamine is a double-edged sword. You need it to survive and function effectively, but it must be precisely controlled. Think of it like a fire alarm system.
Histamine’s Essential Roles: How Your Body Uses It Correctly
When everything is working right, histamine is a crucial messenger. It has different jobs depending on where it’s released:
In your immune system, it’s part of the 911 call. A bug bite or infection triggers special cells to release histamine at the site, causing swelling, redness, and increased blood flow that signal for help. Think of it as pulling the fire alarm for a single room.
In your brain, it acts like a natural cup of coffee, promoting wakefulness, alertness, and a healthy sleep-wake cycle.
When you eat, histamine travels to your stomach to flip the “ON” switch for acid production, helping you break down your food properly.
It even helps regulate your blood vessels, fine-tuning your blood pressure and body temperature.
But in histamine intolerance, this precise signaling system fails.
Histamine Overload: When the Alarm Won’t Turn Off
The problem in histamine intolerance isn’t the histamine itself—it’s the volume and location.
The trouble starts when histamine escapes these local zones and floods the entire system. Instead of targeted alarms in specific rooms, it’s like pulling the master fire alarm for the whole building when there’s no major fire.
You’re not allergic to histamine. You have too much of a good thing in the wrong places. It’s a plumbing and volume problem, not a case of mistaken identity.
Therefore, the goal isn’t to eliminate histamine—you can’t and shouldn’t. The goal is to help your body manage it properly, so it acts as a precise messenger, not a system-wide alarm.
The DAO Enzyme: Your Histamine “Drain Plug”
Remember the clogged drain from the overflowing bucket? This is where we meet the body’s maintenance crew.
The key enzyme is diamine oxidase (DAO). Think of DAO as your personal histamine drain plug.
Here’s its full-time job: Patrol your gut, find histamine, and break it down.
Most of the histamine you encounter comes from what you eat and drink. The small intestine is the primary site of digestion. This is exactly where your body stations its DAO enzyme factory.
How Your DAO Enzyme System Should Work:
- You eat a meal that contains some histamine (like a piece of aged cheese or last night’s leftovers).
- As that food travels into your small intestine, specialized cells in your gut lining release the DAO enzyme right into the digestive tract.
- The DAO acts like Pac-Man, metabolizing dietary histamine and breaking it down into harmless fragments before it can be absorbed into the bloodstream.
- Crisis averted. The histamine is neutralized locally, and your “bucket” stays balanced.
The Problem with DAO in Histamine Intolerance:
For many people, this system breaks down. The “drain plug” (DAO) is either missing, broken, or blocked.
- The Factory is Damaged: Chronic gut inflammation, food sensitivities, or infections can injure the gut-lining cells that produce DAO, crippling your enzyme production.
- The Genetic Blueprint is Faulty: Some people inherit genes that instruct the body to produce less DAO or a less effective version from the start.
- The Drain is Blocked: Certain substances—especially alcohol (wine, beer) and common medications (NSAIDs, some antidepressants)—directly inhibit the DAO enzyme, preventing it from working.
When your DAO drain is clogged, histamine from your food isn’t broken down. It enters your bloodstream directly, filling your bucket and causing systemic symptoms.
Understanding your DAO function is essential to addressing histamine intolerance. The strategies that work—from diet changes to specific supplements—all focus on one of two things: reducing the flow from the faucet or, more importantly, fixing, unblocking, and supporting your DAO drain.
Why Is My “Bucket” Overflowing? Root Cause Analysis
So your bucket is overflowing. The big question is: Why? What turned the faucet on full blast or clogged your drain?
For most people, it’s not just one thing. It’s a combination of factors that accumulate over time, finally pushing your system past its limits.
Let’s investigate the usual suspects.
Suspect #1: Gut Health is Ground Zero for Histamine Intolerance
Your gut is more than just a food tube; it’s your DAO factory and your first line of defense. When your gut is unhappy, histamine management falls apart.
- The Leaky Pipe (Intestinal Permeability): Think of your gut lining as a tightly woven net. Stress, poor diet, infections, or toxins can rip tiny holes in that net. This “leaky gut” allows too much histamine (and other irritants) to enter your bloodstream, overwhelming your system.
- Bad Roommates (Dysbiosis & SIBO): Your gut is home to trillions of bacteria. Some are beneficial, some are neutral, and some are harmful and can cause histamine release. An overgrowth of these nasty bugs (dysbiosis), especially in your small intestine (SIBO), is like having roommates who keep cranking up the faucet, pouring more and more histamine into your internal bucket.
- Factory Damage: Conditions like untreated celiac disease or IBD (Crohn’s, ulcerative colitis) directly damage the very cells in your gut lining that are supposed to produce the DAO enzyme. It’s like the factory floor has been flooded.
Suspect #2: Your Genetic Blueprint
Some people are simply born with a smaller bucket or a slower drain.
You might inherit genes that instruct your body to make less DAO enzyme or a less effective version of it. This doesn’t mean you’re doomed to have symptoms, but it means your margin for error is smaller. You have to be more careful not to overfill the bucket.
Suspect #3: The Drain Blockers
Even if you generate enough DAO, certain factors can clog the drain and prevent it from working.
- Alcohol (especially wine, beer, and champagne) is a major DAO blocker.
- Common Medications, including many over-the-counter pain relievers (NSAIDs like ibuprofen/Advil) and some antidepressants, can block DAO activity.
Suspect #4: The Internal Alarm System (Mast Cells)
You have specialized immune cells called mast cells distributed throughout your body. Their role is to release histamine (and other chemicals) as an initial alarm response to real threats such as infection.
In some individuals, these mast cells become unstable or overly sensitive—a condition often associated with histamine intolerance, known as Mast Cell Activation Syndrome (MCAS). MCAS is less common and can, in some cases, involve severe systemic reactions that may require emergency medication. If this is not the case, your symptoms are likely due to histamine intolerance or associated conditions such as SIBO, leaky gut, etc., until proven otherwise.
Think of it as a hypersensitive fire alarm. Triggers such as stress, chemicals, infections, or certain foods can cause these cells to release histamine internally, filling your bucket from the inside out.
Suspect #5: The Hormone Connection (Estrogen)
Estrogen naturally stimulates the release of histamine from mast cells.
This is a key reason why women often see their symptoms flare cyclically with their menstrual cycle or experience a significant worsening during perimenopause, when hormones swing wildly. High estrogen levels, or estrogen dominance, can increase histamine levels.
Moreover, histamine also stimulates estrogen production, creating a potential vicious cycle, which further explains the female predominance of histamine-related problems.
Putting It Together:
You might have a genetic tendency (a smaller bucket), combined with a gut infection that damages your DAO production (clogs the drain), and a diet high in aged foods (turns up the faucet).
The goal of a functional approach is to be a detective—to figure out your unique combination of causes, so you can fix the plumbing at its source, not just bail out the bucket forever.
The Wide Range of Histamine Intolerance Symptoms
If histamine intolerance had one obvious symptom, it would be easy to spot. But it doesn’t. Instead, it creates a confusing constellation of symptoms that can seem totally unrelated.
Why? Because histamine receptors are everywhere in your body—in your gut, your brain, your skin, your heart, and your lungs. When too much histamine floods your system, it can trigger alarms in different parts of your body, often simultaneously.
This is why people (and sometimes doctors) get so confused. They treat the headache, then the stomach ache, then the rash, never connecting the dots. Let’s connect them.
Here is the constellation, organized by what part of your body is sounding the alarm:
The Brain & Nerves (Neurological Symptoms)
Histamine’s role as a neurological stimulant goes haywire, leading to headaches and migraines (often after meals), debilitating brain fog, dizziness, unexplained anxiety or panic attacks, and significant sleep disturbances.
The Gut (Gastrointestinal Symptoms)
As a direct gut irritant and stimulant, histamine commonly causes bloating, gas, diarrhea, and abdominal pain that mimics IBS. It can also trigger heartburn, acid reflux (GERD), and nausea by stimulating excess stomach acid.
The Skin (Dermatological Symptoms)
The most visible signs include sudden flushing and redness of the face and chest, random hives and itching, eczema flares, and swelling of the lips or eyelids.
The Heart & Lungs (Cardiovascular & Respiratory Symptoms)
Histamine affects blood vessels and smooth muscle, which can cause a racing heart (tachycardia), low blood pressure leading to dizziness, nasal congestion and sneezing, and asthma-like wheezing or shortness of breath.
The Whole Body (General Symptoms)
System-wide inflammation and overload often result in profound fatigue, menstrual irregularities like worse PMS, and generalized body aches and pains.
The Key Clue: Timing & Triggers.
The most important evidence that these symptoms are histamine-related is their association with triggers. They often flare:
- After meals (especially aged, fermented, or leftover foods)
- After drinking alcohol (wine and beer are the biggest culprits)
- Around your menstrual cycle
- During times of high stress
- After taking certain medications
If you see yourself in this constellation, you’re not imagining things. You’re not a collection of separate, random problems. You’re likely seeing the warning lights of a single overloaded system. Recognizing this pattern is the first powerful step toward taking control.
Who Gets Hit? Common Patient Profiles
Histamine intolerance doesn’t pick its targets at random. While anyone can develop it, certain groups of people are more likely to experience it. Seeing yourself in one of these profiles can be a powerful “aha!” moment.
If you’re dealing with any of the following conditions, histamine intolerance might be the missing piece that explains your stubborn symptoms:
- People with Chronic Gut Conditions already have a diagnosed issue like IBS, SIBO, or IBD. Here’s the connection: histamine is a direct gut irritant, and conditions like SIBO involve bacteria that produce it. Furthermore, chronic gut inflammation from IBD or celiac disease damages the very cells that produce your DAO enzyme, destroying your primary defense.
- People with Hormone-Related Flares (especially women) experience symptoms that coincide with hormonal shifts. Since estrogen stimulates histamine release, those with PMS, PMDD, or in perimenopause often see a dramatic worsening of symptoms. Hormonal medications can also influence these pathways.
- People Under Chronic Stress face a double-edged sword. Long-term stress weakens the gut lining (reducing DAO production) and can directly destabilize mast cells, causing them to release histamine. If you’re burned out, your histamine bucket is likely overflowing.
- People with Complex Chronic Conditions are dealing with a diagnosis like MCAS (Mast Cell Activation Syndrome), Long COVID, ME/CFS, or Ehlers-Danlos Syndrome (EDS). These conditions are frequently linked to histamine issues, either through direct mast cell activation (MCAS) or via the gut damage and inflammation they can cause.
- People with New-Onset Sensitivities may have never had food issues before, but now react to wine, aged cheese, or leftovers. This often points to a new root cause—like a post-infectious case of SIBO, a significant hormonal shift (e.g., perimenopause), or a major stress event that damaged the gut lining and DAO production.
Why This Matters:
Being here isn’t about obtaining another label. It’s about finding a direction. If you have IBS, just treating the IBS might not work if histamine is the real trigger. If you have hormone-related symptoms, balancing hormones may fail if you don’t also address any histamine overload.
Understanding your profile helps you and your practitioner connect the dots and create a plan that hits the root cause, not just the symptoms.
How Is Histamine Intolerance Diagnosed? The Functional Medicine Detective Work
Here’s the frustrating truth: there’s no single, simple test that definitively says, “You have histamine intolerance.” Your primary care physician might order allergy tests (often negative) and basic blood work (often normal), leaving you feeling dismissed.
Functional medicine takes a different approach. It acts like a detective, piecing together clues from your story, your symptoms, and strategic tests to build a clear case. The diagnosis rests on a three-part investigation.
The First Clue: Your Symptom & Food Diary
You become the primary investigator. This low-tech tool is incredibly powerful. For 2-4 weeks, meticulously track what you eat, your stress levels, and all symptoms. The goal is to spot clear patterns: Do symptoms flare 90 minutes to 4 hours after aged cheese or wine? Do they worsen before your period? This self-collected data is often the strongest initial evidence.
The Gold Standard: The Elimination Diet
Think of this as a definitive experiment you conduct on yourself. For 3-4 weeks, you strictly avoid all high-histamine foods and DAO blockers (like alcohol). The goal is to reduce your histamine load and assess whether your symptom constellation improves significantly. After this reset, you systematically “challenge” your body by reintroducing one high-histamine food at a time. If symptoms vanish on the diet and return when challenged, you have direct evidence of a dietary link.
Finding the “Why” Behind Histamine Intolerance: Functional Lab Tests
While they don’t directly diagnose intolerance, targeted tests are crucial for uncovering the root cause. A DAO Blood Test can reveal if your enzyme activity is low. A Comprehensive Stool Test looks for gut dysbiosis, histamine-producing bacteria, signs of SIBO, and “leaky gut”—all of which can destroy your DAO production.
Depending on your history, a practitioner may also recommend tests for SIBO (breath test), hormone imbalances (blood, urine, or saliva), or relevant genetic variants (cheek swab, DAO & HNMT).
DAO is the gene that codes for the enzyme that breaks down histamine in the gut, before histamine can be absorbed into the bloodstream. HNMT codes the enzyme that breaks down histamine elsewhere in the body, such as in the brain, skin, and lungs.
If you have “slow” copies of these genes, your ability to break down histamine in the body is less, giving you a smaller bucket for histamine symptoms to develop.
Putting the Case Together
A functional medicine practitioner synthesizes this evidence: your personal history, the results of your elimination diet experiment, and relevant lab findings. The diagnosis is confirmed when a clear picture emerges: you have a consistent set of histamine-triggered symptoms, and identifiable root causes explain why your body’s management system failed.
This process moves you from a state of mystery and frustration to one of clarity and empowerment. You’re not “making it up”—you’ve collected the evidence. Now, you can move on to the solution phase with a targeted plan.
Navigating Solutions: Core Strategies for Histamine Intolerance Management
Successfully managing histamine intolerance requires a multifaceted approach that addresses both immediate symptoms and underlying causes. There is no single “protocol” that works for everyone; rather, a toolkit of strategies that can be personalized. The most effective plans typically involve a combination of dietary modification, gut healing, and strategic supplementation, implemented in a logical sequence.
Dietary Management: Your Foundational Tool
Dietary intervention is the most direct way to reduce the histamine load entering your system—it’s how you “turn down the faucet.”
The Low-Histamine Elimination Approach
A temporary period of strict dietary modification is often the first and most powerful step. This is not meant to be a permanent way of eating, but a 2-4 week “reset” designed to lower your overall histamine burden, calm inflammation, and provide clear symptom relief. This establishes a critical baseline of wellness.
Key Dietary Principles:
- Prioritize Freshness: Histamine levels in food increase with time due to bacterial activity. The most important rule is to choose foods you can cook and eat fresh.
- Handle Leftovers Strategically: If you save cooked food, freeze it immediately to pause bacterial growth. Reheat from frozen, and avoid storing cooked meats or meals in the refrigerator for more than 24 hours.
- Avoid High-Histamine & DAO-Blocking Foods: The core of the elimination phase involves removing major dietary sources of histamine and DAO-blocking foods.
Common High-Histamine Foods to Limit During an Elimination Reset:
| Category | Examples to Limit/Avoid |
|---|---|
| Aged & Fermented Foods | Aged cheeses (parmesan, cheddar), yogurt, kefir, kombucha, sauerkraut, soy sauce, vinegar. |
| Processed & Cured Meats | Salami, pepperoni, bacon, hot dogs, smoked fish. |
| Alcohol | Wine, beer, and champagne are particularly high in histamine and are DAO blockers. |
| Certain Fruits & Vegetables | Spinach, tomatoes, eggplant, avocado. Citrus, strawberries, bananas, pineapple. |
| Leftovers | Meat, fish, or poultry stored in the fridge. |
| DAO Blockers | Black tea, green tea, energy drinks. |
The Reintroduction & Personalization Phase
After a period of symptom stability (often 3-4 weeks), the elimination diet transitions into its most important phase: systematic reintroduction. This is how you move from a restrictive list to a personalized, sustainable diet.
Goal: To identify your unique triggers and tolerance levels. You may find you can tolerate cheddar but not wine, or fresh tomato but not spinach. This knowledge is empowering and removes the fear of food.
Method: Test one high-histamine food at a time, in a small amount, and monitor for symptoms for 48-72 hours.
A Functional Roadmap for Gut Healing & Systemic Support
Beyond diet, addressing gut health—where your primary histamine-degrading enzyme (DAO) is produced—is crucial for long-term resilience. This work often follows a logical progression.
Initial Focus: Crisis Management & Gut Lining Support
The first stage of intervention focuses on reducing the acute histamine load and initiating repair of the intestinal lining, which is often compromised.
- Dietary Foundation: Implementing the low-histamine elimination diet.
- Gut Repair Nutrients: Introduction of foundational supplements like L-Glutamine and Zinc Carnosine, which provide direct support to the gut lining cells that produce DAO.
- Bind Gut Irritants: Supplemental immunoglobulins bind leaky gut toxins before they can be absorbed into the bloodstream – supporting inflammation and immune balance. I like MegaIgG2000 by Microbiome Labs.
- Direct Enzyme Support: Use of a supplemental DAO enzyme taken before meals can provide immediate, temporary relief by breaking down dietary histamine directly in the digestive tract, acting as an external “drain crew.”
For example, you want a supplement with a clinically relevant dose, such as one providing 30,000 to 40,000 HDU per capsule. A product like Histamine Digest by Diem, available in both a 30,000 HDU formula and a 40,000 HDU Histamine Digest Puremax version, is designed to provide this level of effective mealtime support.
Secondary Focus: Addressing Root Causes & Stability
Once symptoms are calmer, the focus can shift to supporting the body’s internal systems and addressing dysbiosis.
- Mast Cell Stabilization: For those with symptoms driven by reactive mast cells (e.g., flushing, itching, anxiety), natural stabilizers such as Quercetin, Luteolin, Rutin, and Vitamin C can help calm histamine release triggered by these cells.
Quercetin is a potent flavonoid and the best-known natural mast cell stabilizer. It helps inhibit the release of histamine and other inflammatory mediators from mast cells. For best absorption and effect, it’s often paired with Vitamin C and Bromelain (a pineapple enzyme), such as in Quercetin Bromelain Forte by SFI Health.
I use a more bioavailable form of quercetin called isoquercitrin. I use Isoquercitin by US Enzymes.
Luteolin and rutin are also potent flavonoids that support mast-cell stabilization and inflammation. Quercetin Bioflavonoids by Allergy Research Group contains both of these (luteolin is a component of lemon bioflavonoids).
Vitamin C is a foundational nutrient that also functions as a natural antihistamine and mast cell stabilizer. I like Vitamin C with Bioflavonoids by Vital Nutrients - Supporting Your Body’s DAO Enzyme: Your body’s own production and function of the DAO enzyme depends on specific nutrients. Activated Vitamin B6 (Pyridoxal-5-Phosphate or P-5-P) is a direct and essential cofactor for DAO. A high-quality Methylated B-Complex can provide this in its active form while also supporting overall methylation, a foundational biochemical process. I use Opti-Absorb B-Complex by Doctor Alex Supplements.
- Supporting the HNMT Pathway (For Neurological & Systemic Symptoms): Histamine inside cells—such as in the brain, skin, and lungs—is broken down by a different enzyme called HNMT. This enzyme is directly dependent on S-adenosyl methionine (SAM-e) as its methyl donor.
While a methylated B-complex supports the methylation cycle that produces SAM-e, targeted SAM-e supplementation may be necessary to directly and effectively support HNMT activity, particularly for stubborn neurological symptoms like brain fog or headaches.
Dosing SAM-e can require professional guidance, especially if you are on medications such as serotonin drugs. I use SAM-e 200 mg by Metabolic Maintenance. - Careful Microbiome Support: Reinoculating the gut is a critical but delicate step, as many common probiotic strains can directly worsen symptoms. Strains such as Lactobacillus casei and Lactobacillus bulgaricus harbor genes that enable them to produce histamine, thereby increasing the internal load.
The strategy is to select probiotic strains that are histamine-neutral or histamine-degrading. While many strains do not produce histamine, some of my research-supported favorites include:
–Spore-forming probiotics (e.g., Bacillus species)
–Specific Bifidobacterium strains (e.g., B. infantis, B. longum)
–Lactobacillus rhamnosus GG
–Saccharomyces boulardii (a beneficial yeast)
My favorite products here include Megasporebiotic, TrubifidoPRO, Epic Defense, and RestorFlora.
Long-Term Focus: Personalization, Resilience & The Setback Mindset
Management evolves into a flexible, long-term practice focused on understanding your unique body.
- Personalized Diet: Using your reintroduction data to create a varied, sustainable diet.
- Dynamic Supplement Use: Transitioning supplements from daily use to strategic support (e.g., DAO enzymes for risky meals, mast cell stabilizers during high-stress periods).
- Mastering Setbacks: Expect fluctuations—they’re data, not failure. Your proactive flare plan:
1) Pause (return to Phase 1 safe foods/core supports)
2) Investigate (review triggers from the prior 72 hours)
3) Recover (support gut healing with gentle nourishment). - Understanding Your Capacity: Recognizing that your “histamine bucket” size is dynamic. Being mindful of natural hormonal cycles and periods of high stress helps you adjust your strategy in real time to maintain balance.
Empowerment and Your Path Forward
Histamine intolerance is complex, but it is not a life sentence. By understanding the “bucket” analogy and learning how to apply these core strategies—turning down the faucet (diet), unclogging the drain (gut healing & DAO support), and stabilizing the internal alarms (mast cell & HNMT support)—you take back control.
Related Articles: